
Vertebral Compression Fracture and Kyphoplasty
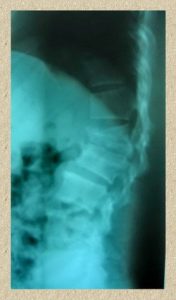
Why suffer from chronic back pain caused by back injuries, trauma and osteoporosis when you can reverse it without an open surgery?
The Kyphon Kyphoplasty Technique
Around the world, there are 100 million people who are at risk of having thin bones, with a staggering 44 million cases found in the USA alone. The most at risk are women who account for 4 times the amount of cases with more than half of are aged over 55 years old. The medical treatment expense for this issue is 20 million dollars per year, which is an amount that even exceeds the costs involved for the treatment of heart diseases (treatment expenses are made up of the hospital expenses added to the financial loss caused by being unable to attend work whilst recovering).
Thin bones can result in broken bones in more than 1.5 million Americans every year. Among this amount, 700,000 patients are found to have a broken vertebral bone (data from National Osteoporosis Foundation). When the broken back bone is at the upper chest area, the spine will be severely compressed; resulting in the lung volume becoming depressed by 9%. Subsequently, lungs may not function properly and breathing can be seriously affected, especially in the elderly.
For patients with thin bones, seemingly harmless incidents, such as a small fall on the buttock, riding in the car on a bumpy road or making a wrong body turn, can cause a crushed backbone (compression fracture of the spine bone). Alarmingly, the symptoms might not be felt right away and it could take up to 2-3 days or even several weeks for pain to be felt. Furthermore, if left untreated, or the wrong treatment is administered, the pain will gradually increase over time.
Symptoms of a Broken Vertebral Bone
Usually, the symptoms start with a backache and minor pain at the waist. The backbone is formed; (i.e., the bone collapses in height) and the spine angles forward. At this point, it is difficult to live a normal life, with even the simplest tasks, such as getting out of bed, becoming a burden. There are also a number of other difficulties that a patient will encounter, such as pain when bending or twisting, and an inability to walk for long distances. Due to the fact that their quality of life is hindered, people affected are less inclined to use their body unless absolutely necessary. Unfortunately, this only exasperates the problem as the density and the strength of the bone is reduced due to the reduction of its use. The consequence of this is that the remaining vertebrae will crumble down, causing multiple fractures.
There is also a possibility of a more serious condition developing, such as lung disease, due to the reduction of the lung functioning. Subsequently, the death rate is increased by 23-43%.
Note: A vertebral compression fracture is also called VCF. It is usually caused from a collapse or breakdown in one or more bones of your vertebrae. Vertebrae are round, strong bones that are stacked up on top of each other. Your spine is made up of thirty-three vertebrae. The bones stack up in a line that goes down the middle of your back.
Compression fractures of the spine occur when there is too much pressure on the vertebra. The vertebra collapses, and becomes wedge-shaped, instead of round. The bone tissue on the inside of the vertebra may also get crushed and squeezed. Fractures may be mild or severe. They happen most often in the thoracic (middle) and lumbar (lower) parts of the spine.
Treatment Options for a Vertebral Compression Fracture
1.Non-Surgical treatment
Most compression fractures heal with simple remedies of medicine, rest, avoiding activities that exert added strain on the back and by using a special back brace. Usually patients are also given medication to control the pain. However, although medications can help ease pain, they are not designed to heal the fracture. It is important to note that the crushed spine or the angled forward bone will not return to its original condition. Therefore, a patient may have to live with a humped back resulting to reduction in body height. Another drawback of this method is that the healing of the bone can take up to 3-4 months. During this time, a patient’s quality of life can suffer. Furthermore, there is a risk that the other bones will be crushed and will start to cave in. Put in simple terms, this process is like stacks of the stories of a high building – once one is crushed and tilted, the weight will be loaded on one side and can lead to the rest of the stories crumbling down.

2.Surgical Treatment
Open surgery returns bones to the right place by putting them together using wires, pins, plates, or screws. This method helps raise the crushed bone back to its normal height and can also help lift the humped back. This has been the most common way to address the problem over the last few decades. The advantage of this method is that the crushed bone is ‘lifted up’ so that it does not compress the nerve. Therefore the nerve is not destroyed and can return to its previous state. The drawback is that the patient will lose a small amount of blood, and will encounter pain around the wound, at the skin and around their muscles. Unfortunately, the result on the patient with thin bones is not as effective. Also, this method cannot be performed on a patient with a separate ongoing disease as it is considered too invasive and there is a poor outcome in the osteoporotic bone

3.Vertebroplasty
Vertebroplasty is the procedure for stabilizing compression fractures in the spine. Bone cement is injected into back bones (vertebrae) that have cracked or broken, often because of osteoporosis. The cement hardens, stabilizing the fractures to support your spine. To perform vertebroplasty, the surgeon inserts a needle into the damaged vertebra. Once the surgeon is sure the needle is in the right place, bone cement is injected through the needle into the fractured bone. A reaction in the cement then causes it to harden. This fixes the bone in place so that it does not collapse any further, as it heals. This procedure is most helpful for reducing pain. It also strengthens the fractured bone, which enables patients to rehabilitate faster. The drawback is that the cement might leak out and therefore might not be able to support the crushed bone back in its place.
Note: The cement is not a common constructive cement. Known as polymethylmethacrylate (PMMA), it is a special kind of cement that starts as liquid and hardens over time.
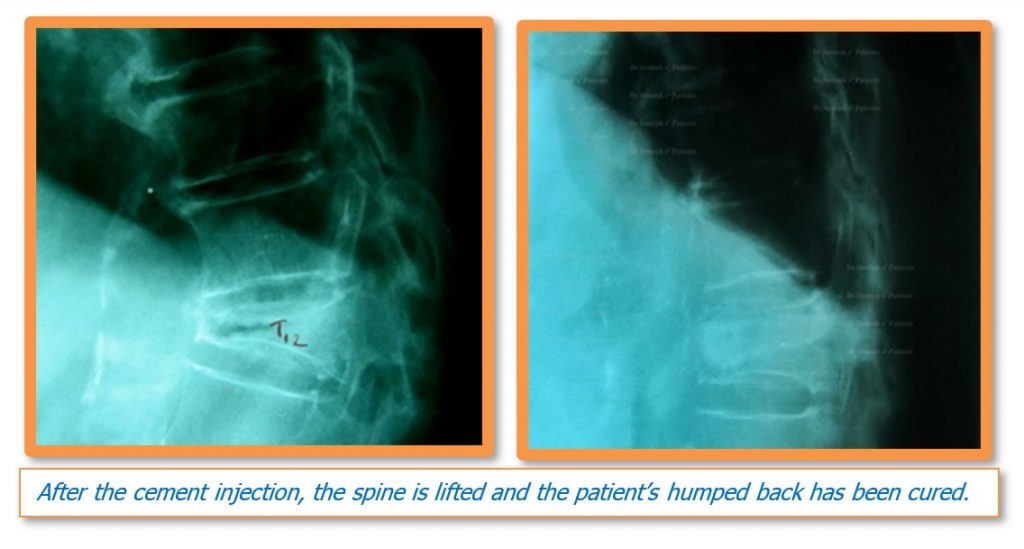
4. Kyphoplasty
Kyphoplasty is when a balloon is placed in the fractured vertebrae. During this process, bone cement is put inside the space made by the balloon. Two long needles are then inserted through the sides of the spinal column into the fractured vertebra body. These needles guide the surgeon while they carefully drill two holes into the vertebral body. There is a large element of skill involved in this process as the needles and drill holes need to be placed in the correct area. The surgeon then slides a hollow tube with a deflated balloon on the end through each drill hole. Inflating the balloons restores the height of the vertebral body and corrects the kyphosis deformity. Before the procedure is complete, the surgeon injects bone cement through a small hole in the skin (percutaneously) into the hollow space formed by the balloon. This fixes the bone in its corrected size and position.
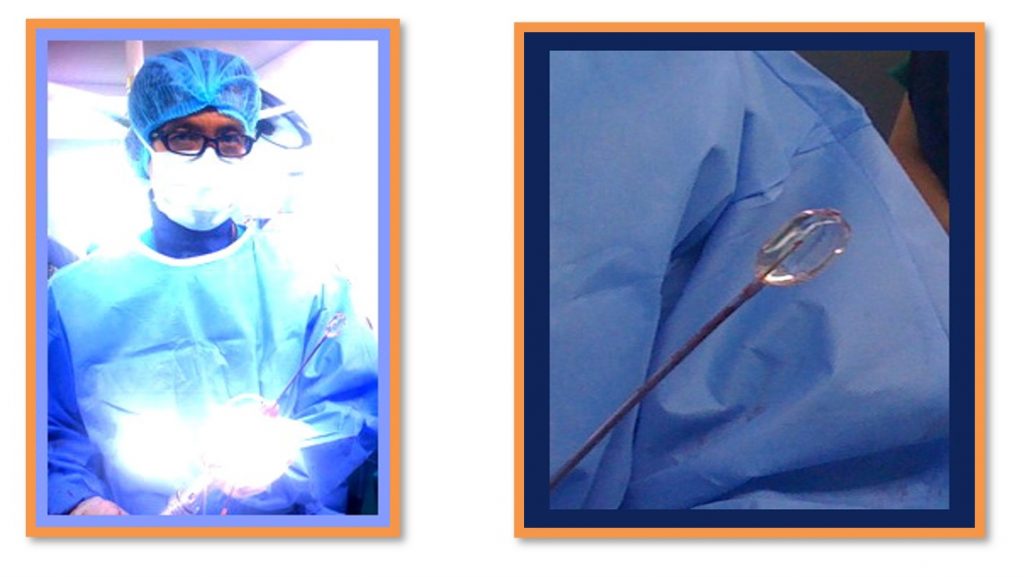
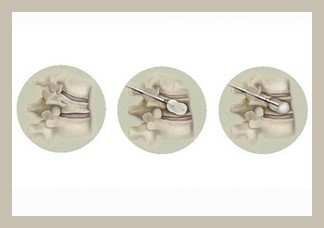
Again, there are advantages and disadvantages of this procedure. One benefit is that no further surgery is required. The procedure also eradicates any severe pain and in fact strengthens the fractured bone. It also gives the advantage of improving some or all of the lost height in the vertebral body. Additionally, the patient will usually recover very quickly; in some cases patients have been known to get up to perform routine activities only a day after the surgery. Furthermore, patients will not need to stay in bed, even during cases, as mentioned previously, when they constantly have to lie down due to the amount of pain caused by body movements. Other advantages are that there will not be a large surgery wound, as well as minimal blood loss for the patient.
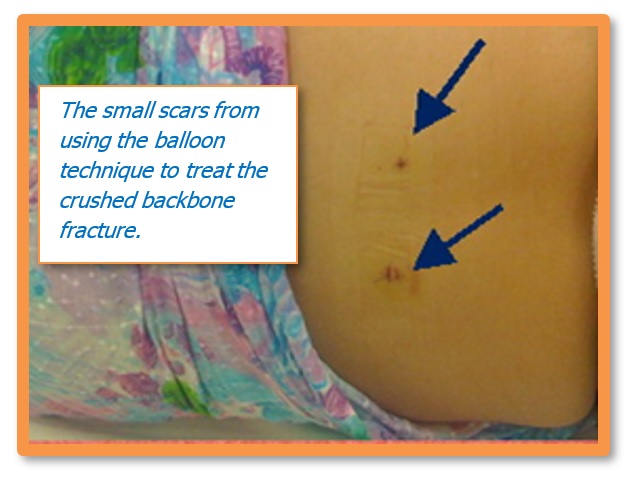
The drawback, however, is that it is an expensive procedure. The equipment and the balloon can only be used once and the surgeon needs to be a skilled specialized doctor who is trained to carry out this type of procedure. In addition to this, the surgeon uses a fluoroscope to guide a needle into the fractured vertebra body. A fluoroscope is a special X-ray television that allows the surgeon to see a patient’s spine and the needle as it moves. As the fluoroscope is not available in every hospital, this can also be costly for the patient.
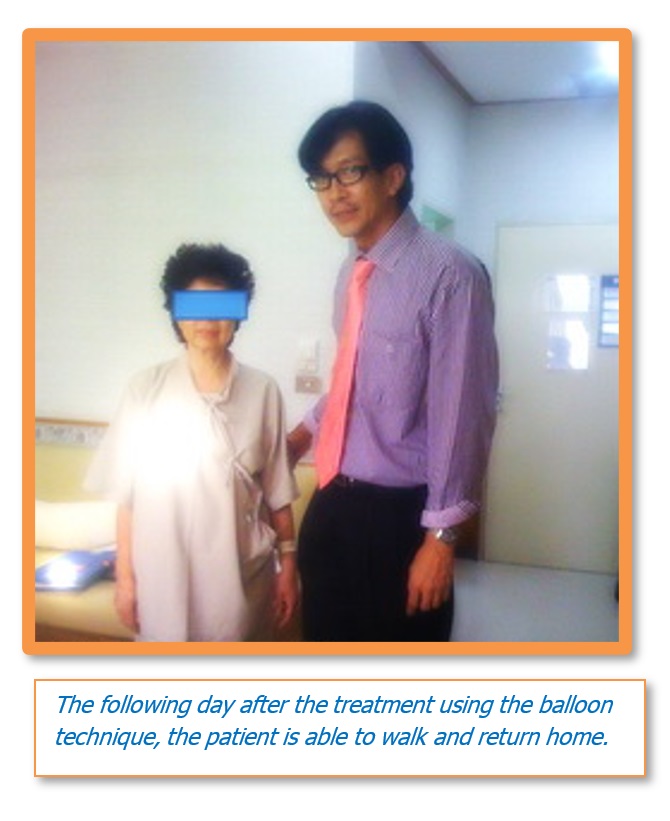
A New Technique in Kyphon Kyophoplasty
From my own observation and experience, in order to make this technique successful within crushed backbone fracture treatment, the following compositions are required:
1.It is essential to use 2 F-x-ray machines in order to see the picture clearly and quickly – this is much more effective than the old technique that uses only 1 machine.

2.Modern, more advanced, pressure measurement equipment is required as it allows for digital measurements and can make finer and more precise calculations, which prevents putting too much pressure in the balloon.
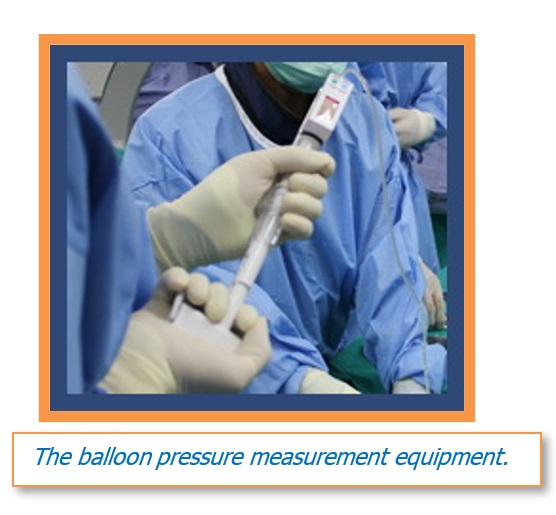
3.The flattened balloon should also be designed for the surgeon to see the point and area to be incised that will ensure greater precision when putting pressure on the area.
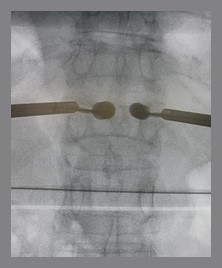
4.When using the new cement injector, it is imperative to make the cement volume and the injection pressure known while the injection is being administered, in order for the injection to be controlled.
Even with these positive recommendations and findings that these techniques are all relatively safe, in reality, there is no single or individual method that is a perfect fit for every patient. The first step should always be to consult your doctor but if possible, it is, of course, much better to keep your bones strong and healthy.
Healthy body and joints to you
RELATED TESTIMONIALS
Mr.Alan Johnson
Khun Wad Mokthaisong
